Back in the spring when the pandemic initially surged around the globe, the places hit the hardest were areas where one would expect a highly contagious respiratory disease to thrive: densely packed, urban metropolises. This makes sense: crowded cities like New York City, where the population density is over 27,000 people per square mile (more than a hundred times the average population density of US metropolitan areas), are clear hotspots where the virus can spread like wildfire.
Remote, rural areas, then, might seem like places that would be less at risk—yet, quite the opposite is true. Rural areas are no more immune to COVID-19 than cities, and, in fact, it’s becoming increasingly clear that rural areas are where the pandemic will hit the hardest and result in the greatest loss of life. The reason is simple: remote, resource-poor, rural areas, unlike urban environments, often lack adequate forms of healthcare support and emergency medical services vital during a crisis like the one we’re in now. These areas often don’t have easy access to PPE, or personal protective equipment, and this is especially true in developing countries where rural communities can be hours away from the nearest hospital.
Recently, my friend Willy Foote, founder and CEO of Root Capital, and I had the opportunity to chat with Dr. Raj Panjabi of Last Mile Health. A luminary at the intersection of medicine and social change, Dr. Panjabi is one of the world’s leading experts in supporting and strengthening rural, community health systems, and has been named by TIME as one of the world’s 100 most influential people and by Fortune as one of the world’s 50 greatest leaders. Between 2013-2016, Dr. Panjabi and his team at Last Mile Health partnered with the Liberian government to spearhead community health efforts that were instrumental in ending the Ebola outbreak.
In our recent webinar, which is available to watch here, we spoke at length with Dr. Panjabi about his experience working with rural leaders, farmer cooperatives, and rural businesses to successfully create and implement systems of trained community healthcare workers that became first-responders and care-givers in the fight against Ebola.By learning from Dr. Panjabi’s experience in Liberia, rural leaders can apply lessons learned from the health worker model in their own communities to fight COVID-19.
We encourage everyone to watch the full webinar for all of Dr. Panjabi’s crucial insights, but here are four key takeaways.
_________________________
1. Promote the 3 W’s: Wear a mask. Wash your hands. Watch your distance.
Whether or not you’re a prominent figure in the community, it’s essential to lead by example and continually remind others of what Dr. Panjabi calls “the 3 W’s”: wear a mask, wash your hands, and watch your distance. But this is especially important if you’re a community leader. As Dr. Panjabi says:
"When a leader who is known to that community, who is trusted by that community, who is loved and admired by that community—when that person puts on a mask, many more people put on masks."
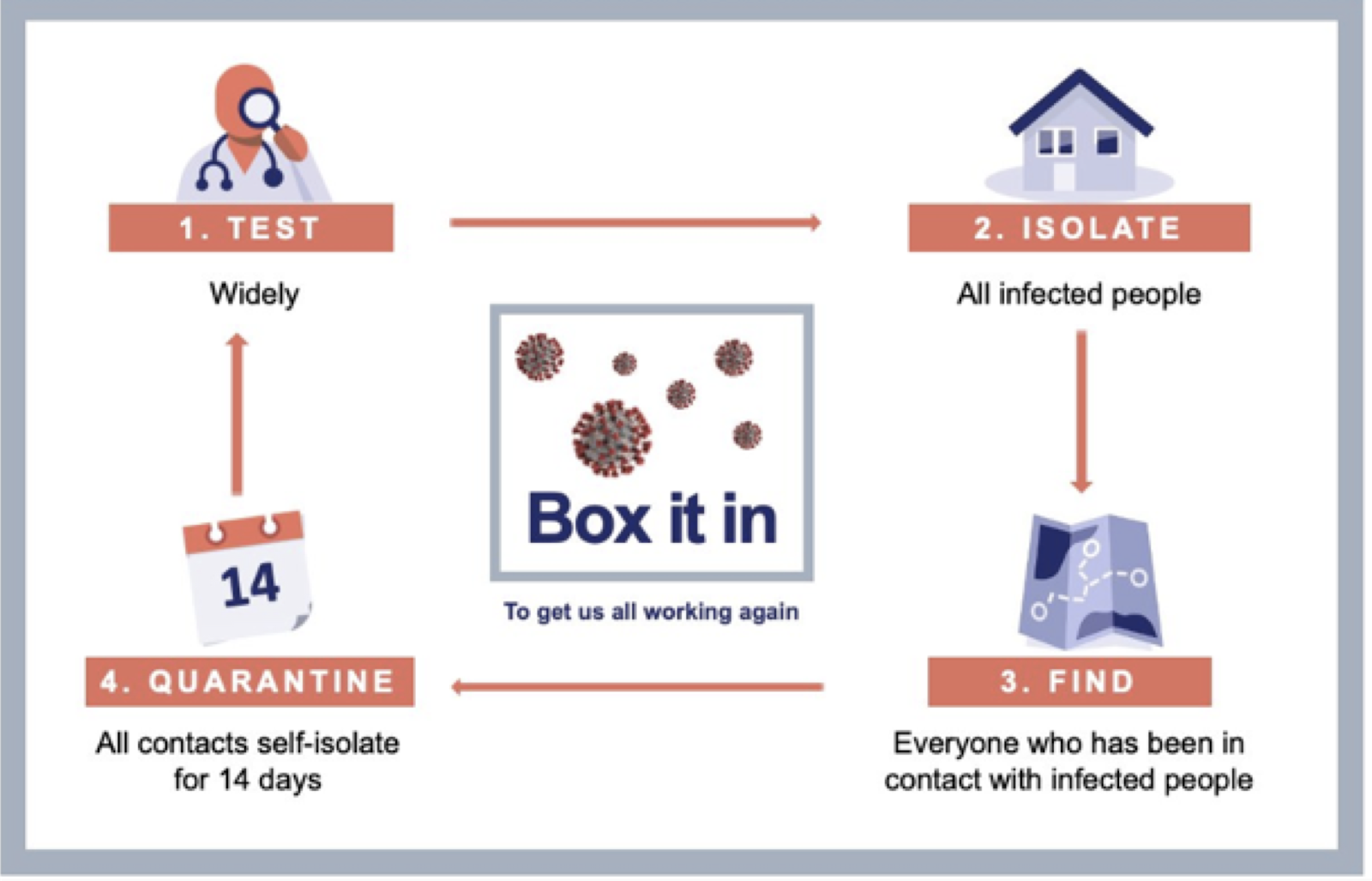 Image credit: Resolve to Save Lives
Image credit: Resolve to Save Lives
Practicing the 3 W’s remains the easiest and most effective way to slow down the spread of COVID-19 and is doable for most people, even those with limited resources. After all, doing anything is better than nothing at all.
"You can yourself wear a mask and encourage people to do that. You can distribute masks in your community. You can look up online how to make those masks if you don't have the ability to purchase them. On washing your hands—water can be a luxury in many rural communities. We know that first-hand. Constructing wells may be a tough thing to do in the middle of this crisis, but it's something that needs to be done for the long-term and that could be a role for businesses to play. Because there will be another pandemic coming. It isn’t just about this one, it’s about becoming more resilient for future ones. We need to put those long-term investments in, but in the short-term—you can still provide chlorinated water and even creek water with soap could eliminate the virus. And on watching your distance, printing educational posters can be critical."
2. Stop the spread of misinformation
"Stop the spread of rumors. If you hear wrong messages, call them out. And then help educate people on the right message."
Spreading wrong information about COVID-19 can be just as harmful as spreading the disease itself. During a time of panic, stress and uncertainty, it can be appealing to cling to theories, rumors, and misinformation that paint the situation in a better light, making it seem not as serious as it really is. For example, claims that masks are harmful and you shouldn’t wear one (they aren’t and you should), that the virus will miraculously disappear (it won’t), or that COVID-19 is “just the flu” (it isn’t) will ultimately cause people to lower their guard and put themselves and others at risk of contracting the virus.
At the same time, it can be tough for many to know who to turn to. But the answer is clear: we need to listen to experts. And by experts, we mean doctors like Dr. Panjabi, organizations like the World Health Organization and the CDC, healthcare professionals who are on the frontlines dealing with COVID-19 every day, and qualified scientists researching the disease and working to develop a vaccine.
Check out the COVID-19 Digital Classroom, a resource put together by Last Mile Health that you can use to educate yourself on COVID-19.
3. Support the sick
“Support those who are sick. Think about what you and your business can be doing to help improve testing, to help ensure those who are sick are isolated and supported, to make sure those who are very sick are transported to hospitals.”
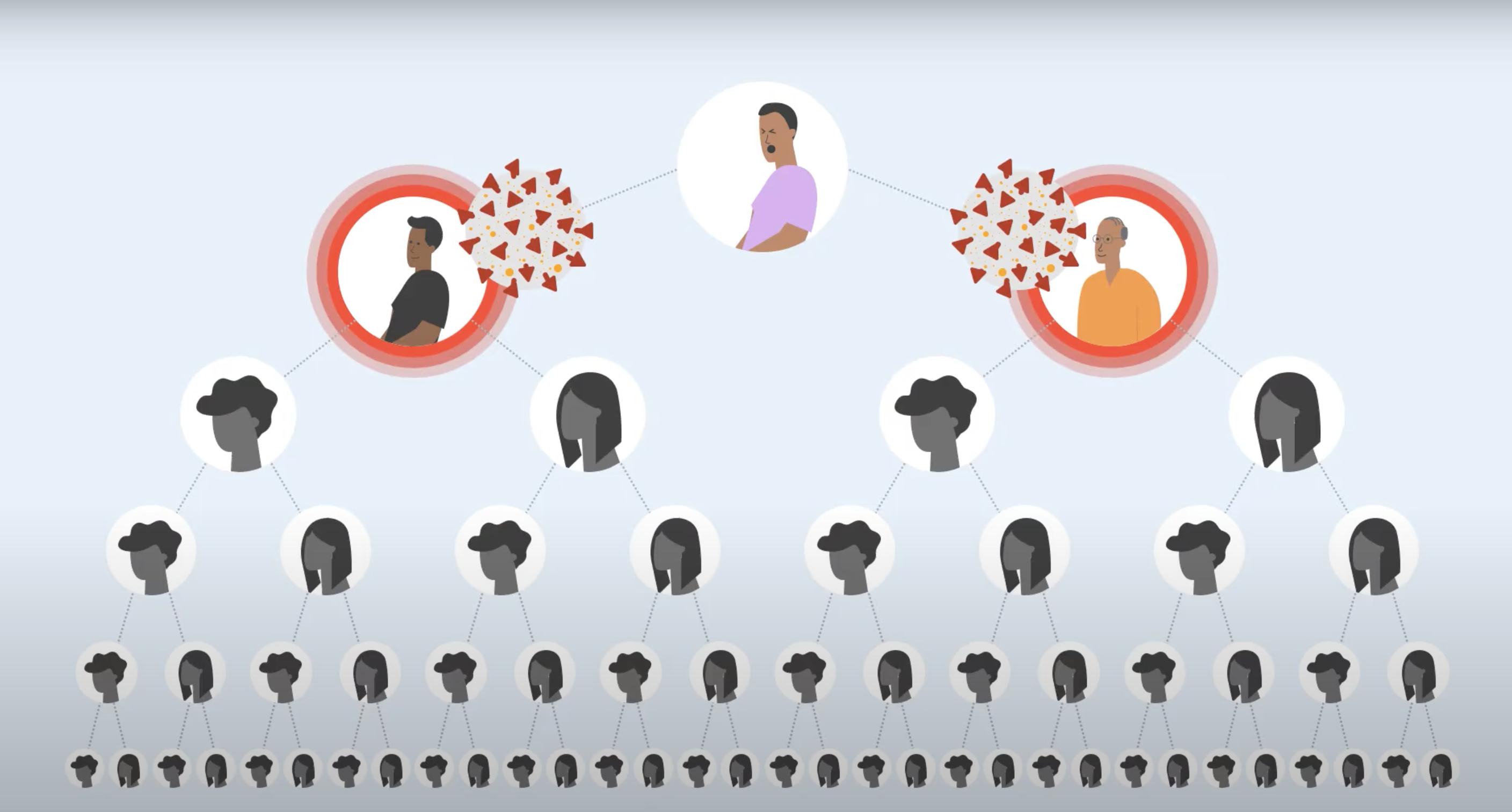
If you or your business are in a position to do so, get in touch with your local government or local health authorities to see how you can be involved in administering and distributing tests. Also see how you can be involved in contact tracing, which will be crucial to breaking the chain of transmission and limiting the spread of new infections. You can learn more about contact tracing in this video.
If there are people in your community who are sick, these people will need to be isolated. While isolated, they’ll need access to food and supplies—consider putting together a system to safely distribute “relief kits” containing food, PPE, and cleaning supplies. In fact, Sustainable Harvest and our partners were able to support farmer cooperatives throughout Latin America and Africa who had already set up distribution systems for these relief kits. These cooperatives were able to leverage their network of farmers in order to get supplies to those most in need. You can read about those efforts here.
4. Be an advocate for community health
"The long term solution here is to make sure that healthcare workers in our rural communities are within reach, that we don't have communities that are out of reach of healthcare. There are still a billion people who live in rural communities who don’t ever see a healthcare worker in their entire lives and go prematurely to their grave.
COVID-19 is the pandemic we’re all focused on right now. But we all know the everyday epidemics: the complications of childbirth, the child with pneumonia who could have gotten antibiotics. These are things that can be prevented, but we cannot do that without providers in place to administer care. A vaccine for COVID-19 is going to be made available—maybe several—in the next 6-12 months. I’m less worried about the vaccine being available than I am about the vaccine getting to all the people that need it. One of the things we need to do is have those providers in place who can administer the vaccine to your own communities.”
If there’s anything that this pandemic has shown us, it’s that we’re all in this together—and we’ll need each other to get out of it. Building a system for community healthcare won’t be easy, but Dr. Panjabi and his team at Last Mile Health have certainly shown it can be done and that it is doable.




.png)
